According to the Centers for Disease Control and Prevention (CDC), obesity rates in America continued rising sharply during the 20 years between 1980 to 2000 with adult rates doubling and children’s rates more than tripling during that time.
New data contained in the “2015 State of Obesity Report: Better Policies for a Healthier America” report (formerly known as “F as in Fat”), produced by the Robert Wood Johnson Foundation (RWJF) and Trust for America’s Health(TFAH), contains analysis is based on data from the CDC’s Behavioral Risk Factor Surveillance System. showing that obesity now puts some 78 million Americans at an increased risk for a range of health problems, including heart disease, diabetes and cancer.
According to the most recent data released September 15, 2015, rates of obesity are highest in the South and Midwest, and nine of the 10 states with the highest rates of diabetes are also in the South. Diabetes rates increased over the past year in eight states: Colorado, Hawaii, Kansas, Massachusetts, Missouri, Montana, Ohio and Pennsylvania.
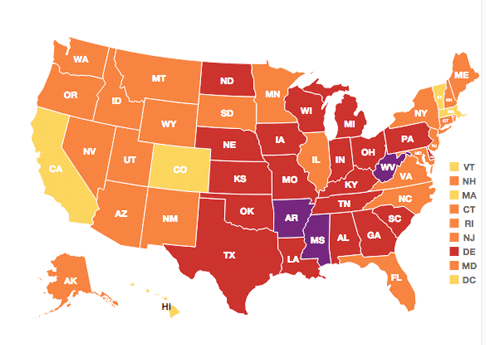 The 12th annual report finds Arkansas with the highest adult obesity rate at 35.9 percent, while Colorado had the lowest at 21.3 percent. Rates of obesity now exceed 35 percent in three states (Arkansas, West Virginia and Mississippi), are at or above 30 percent in 22 states, and are not below 21 percent in any. Seven of the 10 states with the highest obesity rates are in the South and 23 of the 25 states with the highest rates of obesity are in the South and Midwest.
The 12th annual report finds Arkansas with the highest adult obesity rate at 35.9 percent, while Colorado had the lowest at 21.3 percent. Rates of obesity now exceed 35 percent in three states (Arkansas, West Virginia and Mississippi), are at or above 30 percent in 22 states, and are not below 21 percent in any. Seven of the 10 states with the highest obesity rates are in the South and 23 of the 25 states with the highest rates of obesity are in the South and Midwest.
For some recent historical perspective, in 1980, no state had an obesity rate above 15 percent, and in 1991, no state had a rate above 20. In 2000, no state was over 25 percent; and, in 2007, only Mississippi was above 30 percent. Now, nationally, more than 30 percent of adults, nearly 17 percent of 2 to 19 year olds, and more than eight percent of children ages 2 to 5 are obese. The trend line couldn’t be clearer.
The 2015 report notes that starting around 2000, with growing recognition of the epidemic, there have been important inroads made toward preventing and reducing obesity. However, the authors observe that change has been slow and obesity rates remain stubbornly high.
“Efforts to prevent and reduce obesity over the past decade have made a difference. Stabilizing rates is an accomplishment. However, given the continued high rates, it isn’t time to celebrate,” says TFAH executive director Jeffrey Levi, PhD, in a release. “We’ve learned that if we invest in effective programs, we can see signs of progress. But, we still haven’t invested enough to really tip the scales yet.” Dr. Levi oversees TFAH’s work on a range of public health policy issues, including implementation of the public health provisions of the Affordable Care Act and annual reports assessing the nation’s public health preparedness, investment in public health infrastructure, and response to chronic diseases such as obesity. In January 2011, President Obama appointed Dr. Levi to serve as a member of the Advisory Group on Prevention, Health Promotion, and Integrative and Public Health Dr. Levi is also Professor of Health Policy at the Milken Institute School of Public Health at the George Washington University, where his research has focused on HIV/AIDS, Medicaid, and integrating public health with the healthcare delivery system.
Healthy communities characteristically help people lead healthier lives, and small changes that make it easier and more affordable to buy healthy foods and beverages and be physically active can lead to big differences. The U.S. Centers for Disease Control and Prevention, The New York Academy of Medicine, and other experts have identified a range of policies and programs (e.g., improving school nutrition, physical activity and lifestyle interventions, health screenings, walking programs) that can help create healthier communities. Obviously, lower-income communities will typically face higher hurdles, and need more targeted efforts.
RELATED : ORBERA Intragastric Balloon Non-Surgical Weight Loss Device Receives FDA Approval
The obesity phenomenon is attributable to cultural, economic, and sociological changes in communities, neighborhoods and schools that are making it difficult for children to eat healthy diets and to be sufficiently physically active. Straitened economic circumstances result in many families not having access to affordable healthy foods or safe places for kids to walk, bike and play.
Meanwhile, many schools (and homes) across the country continue to make junk food and sugary drinks widely available, while physical education has been increasingly squeezed out of school curriculums. Those factors combined with the vastly greater amount of screen time children nowadays spend preoccupied with texting, social networking, digital gaming, watching movies and other video media, have created a perfect storm of obesity-conducive conditions and factors impacting the nation’s public health, and contributed to the epidemic of childhood obesity.
While obesity rates have increased dramatically among all age groups since 1970, they’ve more than quadrupled among children ages 6 to 11.Today, more than 23 million children and teens in the United States — nearly one in three young people — are overweight or obese, with lower-income communities and communities of color disproportionately affected by the epidemic.
Nationally, obesity rates are 38 percent higher among Blacks than Whites; and more than 26 percent higher among Latinos than Whites (Obesity rates for Blacks: 47.8 percent; Latinos: 42.5 percent; and Whites: 32.6 percent). American Indian/Alaska Natives have the highest adult obesity rate, 54 percent, of any racial or ethnic group. Adult obesity rates are at or above 40 percent for Blacks in 14 states, and at or above 30 percent in 42 states for Blacks; 30 states for Latinos; and 13 states for Whites. Among children and teens (2 to 19 years old), 22.5 percent of Latinos, more than 20 percent of Blacks and 14.1 percent of Whites are obese.
According to CDC data, the rate of obesity among preschool children ages 2 to 5, increased from 5 percent to 10.4 percent between 1976 — 1980 and 2007 — 2008. Obesity rates also increased dramatically among 6- to 11-year-olds (from 4.2% to 19.6% between 1963 – 1965 and 2007 – 2008) and among 12- to 19-year-olds (from 4.6% to 18.1% between 1966 – 1970 and 2007 – 2008).
Obesity prevention among children is key. It is easier and more effective to prevent overweight and obesity in children by particularly focusing on helping every child maintain a healthy weight than it is to reverse trends later. The biggest dividends are gained by starting in early childhood, promoting good nutrition and physical activity so c children enter kindergarten at a healthy weight and healthy habits established for life. The report cites former Surgeon General David Satcher observing that on one level, the problem is simple. Americans continue to eat too much, especially foods with excess calories and few nutrients, don’t get enough physical activity, and spend too much time in our cars and/or in front of our various digital screens.
Compounding the problem is healthy, affordable foods often being more expensive and scarce in many homes and neighborhoods, while sugary, salty, and fatty processed foods are widely available, providing cheap flavor and mouth feel that also cater to development of unsophisticated popular taste culturally conditioned to regard eating vegetables like broccoli or Brussels Sprouts as a punishment rather than a pleasure.
The report cites developing evidence suggesting a link between access to healthy, nutritious foods and academic achievement, noting that students who skip breakfast; are deficient in consumption of fruits, vegetables and dairy products; and are hungry due to insufficient food intake or have deficiencies particularly in key nutrients like Vitamins A, B6, B12, C, folate, iron, and zinc are more likely to have decreased cognitive performances, lower grades, higher rates of absenteeism and tardiness and are unable to focus in the classroom.
The report authors say that reversing the obesity epidemic will require individuals, families, schools, communities, businesses, government, and every other sector of American society to reduce barriers to healthy eating and active living to foster a Culture of Health that makes healthy choices easier for all Americans — a task much more easily defined than achieved.
The authors observe that childhood obesity threatens the health of young people both in the present and impacts their future potential, noting that compared with their healthy-weight peers, obese youths are at greater risk of developing serious health problems, such as heart disease, hypertension, type 2 diabetes, stroke, cancer, asthma and osteoarthritis. Being overweight or obese can put children at a higher risk for these health problems during childhood and as they age. Obese children also miss more school, suffer greater psychological stress, and are more likely to be obese as adults. Conversely, growing up at a healthy weight can set the stage for lifelong health.
“If we don’t reverse this epidemic, the current generation of young people could be the first in U.S. history to live sicker and die younger than their parents’ generation,” say the authors. “Preventing childhood obesity is critical to protecting the viability of our health care system.”
There are also massive economic costs associated with the obesity epidemic both directly and indirectly. The report notes that childhood obesity is a risk factor for many costly chronic diseases that put a tremendous strain on the health care system — the obesity epidemic estimated to cost America $117 billion per year in direct medical expenses and indirect costs, including lost productivity.
Overweight and obesity in childhood alone are associated with $14.1 billion in additional prescription drug, emergency room and outpatient visit healthcare costs annually. Additionally, obesity contributes an estimated incremental lifetime medical cost of $19,000 per 10-year-old child when compared with a healthy-weight 10-year-old child. Children who are obese also incur higher direct healthcare costs — $194 higher for outpatient visit expenditures, $114 higher prescription drug expenditures and $25 higher emergency room expenditures, based on a two-year Medical Expenditure Panel Survey. Data cited in the report notes that average total annual health cost for a child treated for obesity under private insurance is $3,743, while the average health cost for all children covered by private insurance is $1,108.50
Alarmingly, hospitalizations of children and youths with a diagnosis of obesity nearly doubled between 1999 and 2005, while total costs for children and youths with obesity-related hospitalizations increased from $125.9 million in 2001 to $237.6 million in 2005 (in 2005 dollars).
 In a open letter included in the 2015 State of Obesity in America report, Risa Lavizzo-Mourey, MD, MBA, president and CEO of the Robert Wood Johnson Foundation (RWJF), and Jeffrey Levi, PhD, executive director of the Trust for America’s Health (TFAH) observe:
In a open letter included in the 2015 State of Obesity in America report, Risa Lavizzo-Mourey, MD, MBA, president and CEO of the Robert Wood Johnson Foundation (RWJF), and Jeffrey Levi, PhD, executive director of the Trust for America’s Health (TFAH) observe:
“Obesity is one of the biggest healthcare cost drivers adding up to billions of dollars in preventable spending each year. If we fail to change the course of the nation’s obesity epidemic, the current generation of young people may be the first in American history to live shorter, less healthy lives than their parents.
“The Trust for America’s Health and the Robert Wood Johnson Foundation believe that all children in the United States no matter who they are or where they live should have the chance to grow up at a healthy weight. And, that all adults should have the opportunity to be as healthy as they can be no matter what their weight.”
Changing the trends and beginning to turn the tide of obesity will require a greater focus on prevention, with investment in getting children on the right track early to help them maintain a healthy balance of nutrition and physical activity throughout their lives, focusing on strategies to curb the rise in obesity among adults by making healthy choices easier in people’s daily lives, and placing a higher value on prevention instead of dealing with obesity-related health problems after they happen.
The Robert Wood Johnson Foundation provides grants for projects in the United States and U.S. territories that advance our mission to improve the health and health care of all Americans. In their letter, Drs, Lavizzo-Mourey and Levi note that “In 2007, RWJF made a major investment of $500 million to reverse the childhood obesity epidemic. Since then, we have worked with communities, industry, healthcare, government, schools, child care and families around the country to find ways to make healthy choices easier in our daily lives. We’ve learned a lot about what works to change public policies, improve school and community environments and strengthen industry practices in ways that help promote healthy eating and physical activity.”
Happily, they say they’re seeing encouraging signs of progress, with more school districts, cities, counties and states reporting declines in their childhood obesity rates, including Tennessee; Seminole County, Florida; Lincoln, Nebraska; and the Chetek-Weyerhaeuser school district in Wisconsin, among others over the past year.
“But there is far more to do and we can’t stop now,” they emphasize, noting that troubling inequities such as obesity rates being higher among children of color and families living in poverty continuing to persist and requiring a renewed and intensification of focus.
“This year, RWJF announced an additional commitment of $500 million over the next 10 years to expand efforts to help all children grow up at a healthy weight,” say Drs. Lavizzo-Mourey and Levi. “One of the biggest lessons we’ve learned is the importance of starting off in childhood to set the course and stay on track for a lifetime of better health. Building on key areas of work and progress accomplished, this commitment will focus on five big bets:
• Ensure that all children enter kindergarten at a healthy weight;
• Make a healthy school environment the norm and not the exception across the United States;
• Make physical activity a part of the everyday experience for children and youth;
• Make healthy foods and beverages the affordable, available and desired choice in all neighborhoods and communities; and
• Eliminate the consumption of sugar-sweetened beverages among 0- to 5-year-olds.
“In this year’s State of Obesity report, we ask others to join us in stepping up to reinvigorate the commitment to improve the health of our children. The signs of progress are promising. And the stakes are too high not to push forward.”
The 2015 State of Obesity Report: Better Policies for a Healthier America” report is available at:
http://bit.ly/1YzPgXl
Sources:
Robert Wood Johnson Foundation
Trust for America’s Health
Centers for Disease Control and Prevention (CDC)
2015 State of Obesity Report: Better Policies for a Healthier America
Image Credits:
Robert Wood Johnson Foundation
2015 State of Obesity Report: Better Policies for a Healthier America
